Ladies and Gentlemen, I want to talk to you today about a topic that affects millions of people around the world, but is often overlooked and misunderstood - Sleep Apnea. Are you constantly tired, even after a full night's sleep? Do you snore loudly and wake up gasping for air? These could be warning signs of sleep apnea. But don't worry, you're not alone in this journey. In this article, we'll dive into the depths of sleep apnea, exploring the warning signs, causes, and treatments available to help you get the restful sleep you deserve

Overview
If you're someone who constantly feels exhausted even after a full night's sleep, you might be suffering from sleep apnea. This condition, in which your breathing repeatedly stops and starts, can have serious consequences for your health if left untreated. So, what exactly is sleep apnea? According to MayoClinic, there are three main types of sleep apnea, each with its unique characteristics:
Obstructive Sleep Apnea (OSA): The most common form of sleep apnea is obstructive sleep apnea (OSA). This occurs when the throat muscles relax during sleep, causing a blockage in the airway. As a result, you may experience pauses in breathing and might even snore loudly or gasp for air.
Central Sleep Apnea (CSA): Central sleep apnea (CSA) is a less common type of sleep apnea that happens when the brain doesn't send proper signals to the muscles that control breathing. This can lead to pauses in breathing and can be caused by various medical conditions, including heart failure.
Treatment-Emergent Sleep Apnea (TESA): Treatment-emergent sleep apnea (TESA) is a type of sleep apnea that occurs as a result of treatment for another condition. According to Mayoclinic, this type of sleep apnea can develop in individuals who have been treated for conditions such as obesity or drug addiction. As with OSA, TESA can be accompanied by snoring and pauses in breathing.
If you think you may be suffering from sleep apnea, it's important to seek the help of a healthcare provider. With the right treatment, you can ease your symptoms and reduce the risk of developing heart problems and other complications. So don't ignore the signs, take control of your sleep health today!
Here are common warning Signs:
- Excessive daytime sleepiness
- Loud snoring, Choking or gasping during sleep.
- Awaking frequently at night, feeling restless and tired
- Observed pauses in breathing during sleep
- Morning headache
- Dry mouth or sore throat upon awakening
- Trouble paying attention, staying focused, or remembering things
- Irritability, depression, or mood swings
- Reduced interest in sex

The Consequences of Sleep Apnea
The consequences of sleep apnea, both obstructive sleep apnea (OSA) and central sleep apnea (CSA), can be far-reaching and have a significant impact on one's health. The repeated awakenings and disruptions to sleep result in severe daytime drowsiness, fatigue, irritability, and difficulty concentrating. This can lead to problems such as poor performance in school or work, an increased risk of motor vehicle and workplace accidents, and depression. Moreover, OSA and CSA can put strain on the cardiovascular system, increasing the risk of high blood pressure, heart disease, stroke, irregular heartbeats, and type 2 diabetes. The sleep deprivation of partners can also cause problems in relationships. Furthermore, sleep apnea can complicate certain medicines and surgeries, and people with sleep apnea are at higher risk for liver problems and nonalcoholic fatty liver disease. It's important to seek medical attention if you or someone you know is experiencing the warning signs of sleep apnea.
"Invest in your sleep, it's the foundation of a healthy life."
What Causes Sleep Apnea?
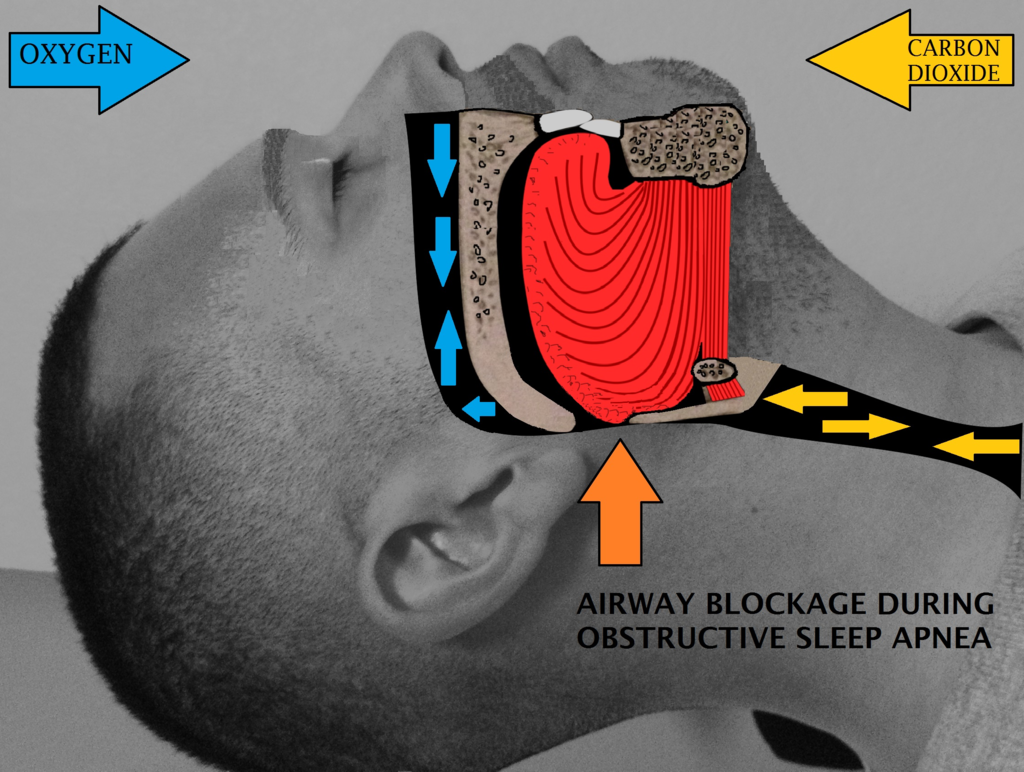
In Obstructive Sleep Apnea (OSA), the airway collapses during sleep as the muscles in the back of the throat relax. These muscles support the soft palate, uvula, tonsils, side walls of the throat, and tongue, and when they become lax, the airway narrows or closes when you inhale.
This leads to a lack of oxygen and a drop in blood oxygen levels, causing your brain to briefly wake you up so that you can open your airway again. This process can repeat itself several times an hour, interrupting deep and restful sleep.
In contrast, Central Sleep Apnea (CSA) is a less common form of sleep apnea that occurs when the brain fails to send signals to the muscles responsible for breathing. As a result, you stop breathing for brief periods and may wake up feeling short of breath or have difficulty falling asleep.
Risk Factors for Sleep Apnea
Sleep apnea can occur in anyone, including children, but there are certain factors that raise the likelihood of developing it.
For Obstructive Sleep Apnea (OSA), the following factors increase the risk:
- Obesity: Excessive weight can lead to fat deposits around the upper airway, obstructing breathing and increasing the risk of OSA.
- Neck size: People with thicker necks might have narrower airways, making it more difficult to breathe.
- Narrow airway: Inherited or genetic factors, such as a narrow throat, enlarged tonsils or adenoids, can contribute to OSA.
- Gender: Men are two to three times more likely to develop sleep apnea, although women's risk increases with obesity or after menopause.
- Age: Sleep apnea is more prevalent in older adults.
- Family history: Having relatives with sleep apnea can increase one's own risk.
- Substance use: Alcohol, sedatives, or tranquilizers can relax the throat muscles, worsening OSA.
- Smoking: Smokers are three times more likely to have OSA than non-smokers, as smoking increases inflammation and fluid buildup in the upper airway.
- Nasal congestion: Difficulty breathing through the nose, whether from a structural issue or allergies, can raise the risk of OSA.
- Health conditions: Certain medical conditions such as congestive heart failure, high blood pressure, and type 2 diabetes can increase the likelihood of OSA, as can hormonal disorders, prior stroke, and chronic lung diseases like asthma.
For Central Sleep Apnea (CSA), the following factors raise the risk:
- Age: Central sleep apnea is more common in middle-aged and older people.
- Gender: Men are more likely to develop CSA than women.
- Heart disorders: Congestive heart failure increases the risk of CSA.
- Pain medicine use: Taking narcotic pain medicines, particularly long-acting ones like methadone, can raise the risk of CSA.
- Stroke history: Having had a stroke increases the risk of central sleep apnea.
How Do Doctors Diagnose Sleep Apnea?
Your healthcare provider may diagnose sleep apnea based on your symptoms and a sleep history. They may also refer you to a sleep disorder center for further evaluation. This evaluation can involve overnight monitoring of your breathing and body functions during sleep at a sleep center or through a home sleep test. Tests for sleep apnea include nocturnal polysomnography and home sleep tests, which monitor heart and lung activity, breathing patterns, blood oxygen levels, and more. If the results are not typical, your provider may prescribe a therapy without additional testing, but further evaluation may still be necessary. If you have obstructive sleep apnea, your provider may refer you to an ear, nose, and throat specialist to check for blockages. A heart specialist or neurologist may also be needed to look for causes of central sleep apnea.
How is Sleep Apnea Treated?
CPAP (Continuous Positive Airway Pressure) is a commonly used machine for those with moderate to severe sleep apnea. This device delivers air pressure through a mask worn while sleeping, maintaining open airway passages and preventing apnea and snoring. Although it's the most reliable form of treatment, some may find it cumbersome or uncomfortable. With time and practice, most people learn to adjust the straps for a secure and comfortable fit, and might need to try various masks before finding the right one
In case using a CPAP machine remains challenging, alternate airway pressure devices like auto-CPAP or BPAP (Bilevel Positive Airway Pressure) are available, automatically adjusting pressure while you sleep. Another option is wearing an oral appliance to keep your throat open, which can be easier to use leading to more compliance but potentially not as effective as the CPAP. A range of devices can be obtained by your Dentist or Over-the-Counter. Regular follow-up appointments with your doctor are necessary to monitor your symptoms.
Surgery for OSA
When it comes to treating obstructive sleep apnea, surgery is often considered a last resort after other treatment options have been exhausted. However, for individuals with specific jaw structure problems, surgery may be the initial course of action. There are several surgical methods that can be considered, such as removing tissues from the back of the mouth, shrinking the tissue in the throat with radiofrequency energy, repositioning the jaw, implanting soft rods into the soft palate, or even stimulating the nerve that controls tongue movement. In some severe cases, a new air passageway may need to be created, known as tracheostomy. If you are considering surgery, it is important to speak with your healthcare provider about the different options and the potential benefits and risks associated with each.

Conclusion
Sleep apnea is a serious condition that should not be taken lightly. Understanding the warning signs, causes, and treatments of sleep apnea is crucial to ensure that those who suffer from it receive the help they need to improve their quality of life. The importance of addressing sleep apnea cannot be overstated, as it can have far-reaching consequences, not just for the individual suffering from it, but also for their loved ones and society as a whole. Just as with any other challenge, we must start by recognizing the problem, and then take the necessary steps to address it. By prioritizing our sleep health, we can all take control of our lives and build a better future for ourselves and those around us. Just like with any other aspect of life, when it comes to sleep apnea, it all starts with a choice. Let's choose to prioritize our sleep health, so that we can live our lives to the fullest.
National Heart, Lung, and Blood Institute (NHLBI) - https://www.nhlbi.nih.gov/
Mayo Clinic - https://www.mayoclinic.org/
The American Sleep Association - https://www.sleepassociation.org/
WebMD - https://www.webmd.com/
Image by <a href="https://www.freepik.com/free-photo/high-angle-uncompleted-checking-boxes_5330507.htm#query=checklist&position=0&from_view=search&track=sph">Freepik</a>boxes_5330507.htm#query=checklist&position=0&from_view=search&track=sph">Freepik</a>





